|
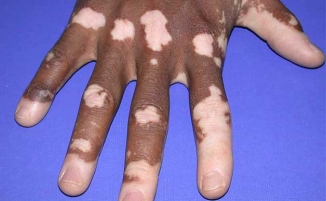
Vitiligo
Vitiligo is a condition that causes depigmentation of sections of skin. It occurs when melanocytes, the cells responsible for skin pigmentation, die or are unable to function. The cause of vitiligo is unknown, but research suggests that it may arise from autoimmune, genetic, oxidative stress, neural, or viral causes. The incidence worldwide is less than 1%. The most common form is non-segmental vitiligo, which tends to appear in symmetric patches, sometimes over large areas of the body.
Clinical features : The most notable symptom of vitiligo is depigmentation of patches of skin that occurs on the extremities. Although patches are initially small, they often enlarge and change shape. When skin lesions occur, they are most prominent on the face, hands and wrists. Depigmentation is particularly noticeable around body orifices, such as the mouth, eyes, nostrils, genitalia and umbilicus.
Types of vitiligo: -Generalized -Focal -Acrofacial -Segmental -Koebner -Mucosal
Treatment of vitiligo:
Medical: · Glucocorticoids, · Immunomodulators “calcineurin inhibitors” (Tacrolimus, pimcrolimus), especially useful on the face and neck where strong steroid creams may cause skin thinning. · Pseudocatalase · topical psoralen.
Phototherapy: Systemic Psorlaen+ UVA (PUVA), UVB-NB/311 Laser therapy: EXCIMER Laser Surgical: Cultured and non-cultured melanocyte transplantation. Coumflage De-pigmenting:In cases of extensive vitiligo (usually > 80%) the option to de-pigment the unaffected skin with topical drugs like monobenzone, mequinol or hydroquinone may be considered to render the skin an even colour. The removal of all the skin pigment with monobenzone is permanent and vigorous. Sun-safety must be adhered to for life to avoid severe sun burn and melanomas. Depigmentation takes about a year to complete.
|